Coming Soon: New Building for Children's Specialty Care
Our new Children's Health Specialty Clinics building will bring 30 pediatric specialties together under one roof, making it easier for families to get expert care.
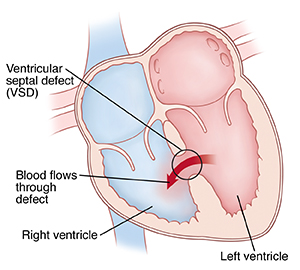
A ventricular septal defect (VSD) is a congenital heart defect. This means that your baby is born with it. A VSD is a hole in the wall (septum) that separates the two lower chambers of the heart (right and left ventricles). VSDs are one of the most common types of congenital heart defects.
The heart has four chambers: two upper (atria) and two lower (ventricles). Blood that is high in oxygen flows from the left atrium to the left ventricle and out to the body, where the vital organs use the oxygen. Blood with less oxygen flows from the right atrium to the right ventricle and out to the lungs. In the lungs, it picks up more oxygen.
Normally, the septal wall prevents the mixing of blood between the two ventricles of the heart. A VSD allows oxygen-rich (red) blood to pass abnormally from the left ventricle through the opening in the septum. Then it mixes with oxygen-poor (blue) blood in the right ventricle.
A large VSD can cause high pressure in the blood vessels in the lungs. The higher pressure can lead to lower oxygen levels in the body. If the VSD is large, your child may need some type of repair. Babies and children with larger VSDs often have symptoms, such as breathing faster and harder than normal. Very small holes in the ventricular septum may not let much blood pass between the ventricles. In these cases, the heart and lungs don’t have to work harder. Sometimes these small holes will close up on their own.
There are different types of VSD. The type your child has depends on which part of the wall between the ventricles is involved. The size of the opening or hole also varies.
VSD may occur more often in some families. This is because of gene problems. Most of the time, healthcare providers don't know the cause of VSD.
Your child may have symptoms from birth. Or your child may not have symptoms until they are a little older. The size of the opening or hole affects how bad your child’s symptoms are. So does the age at which your child first has symptoms. If the hole is small, the only sign may be a heart murmur that your healthcare provider hears with a stethoscope. With a larger opening, the heart and lungs have to work harder.
This can cause symptoms, such as:
Symptoms can occur a bit differently in each child. The symptoms of VSD may also be similar to symptoms of other conditions. Make sure your child sees the healthcare provider for a correct diagnosis.
Your child's healthcare provider may suspect a problem when they hear an abnormal sound (heart murmur) when listening to your child's heart with a stethoscope. If this happens, the healthcare provider may refer your child to a pediatric cardiologist. This is a healthcare provider who specializes in treating heart problems in children.
This provider will check your child and listen to your child’s heart and lungs. The details about the murmur will also help the provider make the diagnosis.
Tests may be needed to confirm the diagnosis. The tests your child has depend on their age and condition, and the provider’s preferences.
A chest X-ray shows the heart and lungs. With a VSD, a chest X-ray may show an enlarged heart. This is because the pulmonary artery, left atrium, and left ventricle get more blood than normal. There may also be changes in the lungs because of extra blood flow.
This test records the electrical activity of the heart. It also shows abnormal rhythms (arrhythmias) and spots heart muscle stress.
An echocardiogram uses sound waves to make a moving picture of the heart and heart valves. This test can show the pattern and amount of blood flow through the septal opening. An echo is used to diagnose VSD.
A cardiac MRI makes images of the body by using magnets and radio waves. It can show the heart defect and how much blood flow is moving through the VSD.
Treatment will depend on your child’s symptoms, age, and general health. It will also depend on how severe the condition is.
A small VSD may close on its own as your child grows. Some small defects don’t close on their own, but they still don’t need treatment. A larger VSD often needs to be fixed with open heart surgery or through procedures during cardiac catheterization. Once a child is diagnosed with a VSD, their pediatric cardiologist will check the defect regularly to see if it’s closing on its own.
Some children may need to take medicine to help the heart work better. Children without symptoms may not need medicine.
Babies with a larger VSD may get tired when feeding. They may not be able to eat enough to gain weight. They may need:
The goal of open heart surgery is to close the septal opening before the lungs are damaged. Surgery will also help babies who have trouble feeding gain a normal amount of weight. Your child's cardiologist will decide when your child should have surgery. This may be based on echocardiogram and cardiac catheterization results. In surgery, your child’s healthcare provider will close the VSD with stitches or a special patch. Talk with your child's healthcare provider for more information.
A VSD may also be fixed during cardiac catheterization. In this procedure, a tool called a septal occluder is used with a catheter. The healthcare provider guides the catheter through the blood vessels to the heart. Once the catheter is in the heart, the provider closes the defect with the septal occluder. Only certain types of VSDs may be closed with this method. This procedure should be done in centers that have staff with experience doing transcatheter VSD repair.
Complications of an untreated VSD include:
Babies with small VSDs may have no symptoms. These children may not need medicine. They’ll still be checked often. If a defect is going to close, it usually happens by age 2. But some defects don’t close until age 4. These children usually grow and develop normally. They also have no activity restrictions and live normal, healthy lives.
If the VSD is moderate to severe, your child will be closely watched. Your child's healthcare provider will decide when and how your child’s VSD will be fixed. Before surgery, your child may need medicine and special feedings. Your child's healthcare team will give you information and support so you can care for them at home. Children who need surgery will be admitted to the hospital for surgery.
Babies who have trouble eating before surgery often have more energy right after surgery. They start to eat better and gain weight faster.
After surgery, older children can often be active without getting too tired. Within a few weeks, your child should be fully recovered. Your child’s healthcare team may give you instructions on how to care for your child.
Most children who have surgery for VSD will live normal, healthy lives. Their activity levels, appetite, and growth often return to normal. Your child may need antibiotics to prevent infections after leaving the hospital.
Ask your child's healthcare provider about your child’s outlook. When this condition is diagnosed early, the outcome is often excellent. The outlook may be poor when a VSD is diagnosed later in life, if complications occur after surgery, or if the VSD isn’t fixed. There is a risk for complications from a VSD. Children at risk for these problems should have follow-up care at a center that specializes in congenital heart disease.
Call the healthcare provider if your child has:
Tips to help you get the most from a visit to your child’s healthcare provider:
Our new Children's Health Specialty Clinics building will bring 30 pediatric specialties together under one roof, making it easier for families to get expert care.